50 year old male with DKA
I’ve been given this case to solve in an attempt to understand the topic of “patient clinical data analysis" to develop my competency in reading and comprehending clinical data including history, clinical findings, investigations, and come up with diagnosis and treatment plan
NAME:- G VISHAL
ROLL NO :- 50
A 42 year old cab driver by occupation presented to OPD with
Chief complaints of
Vomitings since 7 days.
Shortness of breath since 5 days.
History of present illness
Patient was apparently asymptomatic 7 years back then he was diagnosed with Type 2 Diabetes Mellitus, since then he is non complaint to medication of oral hypoglycemic drugs.
7 days back he developed vomiting with 3 episodes per day which is non bilious, non projectile, non foul smelling, food as content without any associating and relieving factors for which he was treated.
No history of stomach pain.
Then he developed shortness of breath 5 days back of grade 4 which is gradual in onset without any associated symptoms like angina, palpitation and hemoptysis for which he was taken to a govt hospital where he was referred to our hospital.
Past history
No history of similar complaints in the past.
H/o Diabetes mellitus since 7 years.
No H/o Hypertension, CAD, asthma, epilepsy, tuberculosis.
No previous history of blood transfusions.
H/o hospital admission 3 years back for food poisoning.
No history of blood transfusions.
Daily routine
Patient wakes up at 6 AM in the morning freshens up drinks tea and has breakfast at around 8:30 AM, goes to work and has lunch at 1:20 PM continues to work drinks tea at 6 PM, dinner at 8:30 PM.
Personal history
Diet is mixed with normal appetite and regular bladder movements, sleep is adequate.
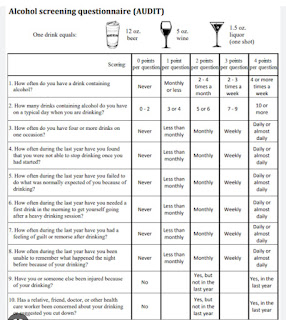
Addictions
Alcoholic since 5 years occasionally
Previous binge is before the onset of vomiting for 5 days 90ml each day.
Skipped meals for 5 days before onset of vomiting.
No drug allergies.
General examination
Patient is conscious, coherent and cooperative, well oriented to time, place and person.
No features indicating the presence of pallor, icterus, cyanosis, clubbing, lymphadenopathy, generalized edema.
Dehydration present at the time of admission - dryness of tongue.

Vitals
Blood pressure 120/70 mmHg
Respiratory rate 24cpm
Pulse rate 82bpm
Temperature febrile
GRBS at the time of admission 464mg/dl
SYSTEMIC EXAMINATION
RS- Bilateral air entry is present, normal vesicular breath sounds heard.
ABDOMINAL EXAMINATION
INSPECTION
Shape - Scaphoid, with no distention.
Umbilicus - Inverted
Equal symmetrical movements in all the quadrants with respiration.
No visible pulsation,peristalsis, dilated veins and localized swellings.
PALPATION
No local rise of temperature
Abdomen is soft with tenderness in the left loin region.
No spleenomegaly, hepatomegaly.
PERCUSSION
Liver span is 12cm.
No hepatomegaly
Fluid thrill and shifting dullness absent.
No puddle sign.
AUSCULTATION
Bowel sounds present.
No bruit or venous hum
CNS examination
Higher motor functions intact
No focal neurological deficits noted.
CVS- S1 and S2 heart sounds heard.
Provisional diagnosis
Diabetic ketoacidosis secondary to non complaint to medication
Diabetes Mellitus type 2 since 7 years
INVESTIGATIONS
Lipid profile
Urine for ketone bodies is positive.
TREATMENT
1. iv normal saline@120ml/hr
2. Inj. Monocef 1gm iv/bd for 6 days
3. inj human actrapid insulin sc/tid
8am. 2pm. 8pm
12u. 12u. 12u
4. inj neutral protamine hagedron(nph) sc/bd
8am. 8pm
16u. 16u
5. Inj pan 40mg iv/od
6. GRBS monitoring 4th hourly.












Comments
Post a Comment